Your web browser is outdated and may be insecure
The RCN recommends using an updated browser such as Microsoft Edge or Google Chrome
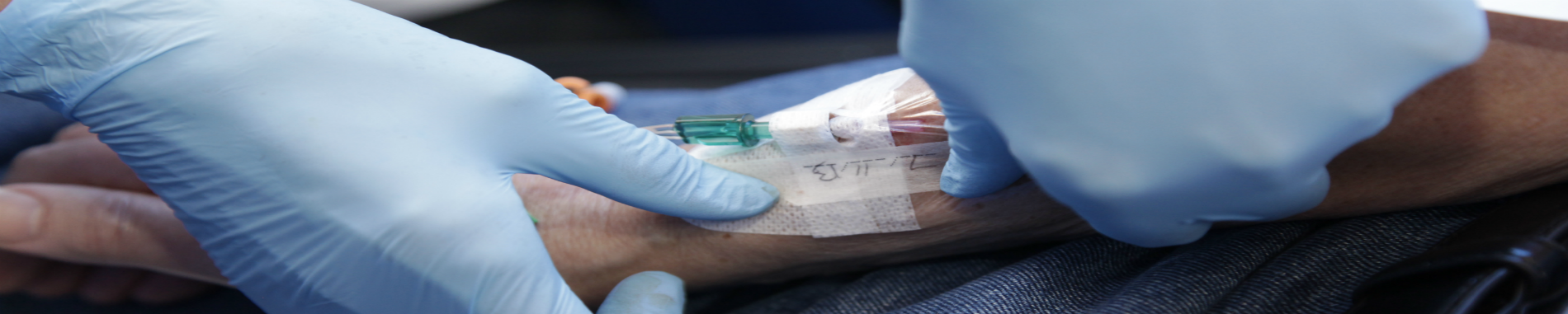

Patient Specific Directions (PSDs) and Patient Group Directions (PGDs)
A patient specific direction (psd) is a written instruction, signed by a prescriber for medicines to be supplied and/or administered to a named patient after the prescriber has assessed the patient on an individual basis., patient group directions (pgds), useful resources.
- Royal Pharmaceutical Society (2019) Professional Guidance on the Administration of Medicines in Healthcare Settings
- Royal Pharmaceutical Society (2019) Practical guide for independent prescribers
- National Institute for Health and Care Excellence (NICE) has published a suite of guidance, advice and support for delivering quality, safety and efficiency in the use of medicines .
- BMA has updated their guidance for Patient Group and Patient Specific Directions . This guidance is for England only.
- CQC Myth buster on Patient Group Directions and Patient Specific Directions
- Medicines and Healthcare products Regulatory Agency (MHRA) regulates medicines, medical devices and blood components for transfusion in the UK.
- MHRA yellow Card Scheme is vital in helping the MHRA monitor the safety of all healthcare products in the UK to ensure they are acceptably safe for patients and users. Reports can be made for all medicines including vaccines, and all medical devices available on the UK market.
- Specialist Pharmacy Service. Influenza vaccine . This includes written instruction templates for adoption.
- Specialist Pharmacy Service. When not to use a PGD . Understanding when PGDs are an unsuitable mechanism for the supply and/or administration of medicines ensures an alternative legal framework is applied.
- Specialist Pharmacy Service. Patient Group Direction use in End of Life Care .
- Specialist Pharmacy Service. Patient Group Direction (PGD) use in a service provided by multiple organisations .
- Specialist Pharmacy Service. Supplying contrast agents under a Patient Group Direction
- Reproductive health national PGDs
- PGD templates to support national immunisation programmes provided on the NHS
- The Role of Nursing Associates in Vaccination and Immunisation. Position statement (April 2019)
- Health Care Support Workers Administering Inactivated Influenza, Shingles and Pneumococcal Vaccines for Adults and Live Attenuated Influenza Vaccine (LAIV) for Children
Page last updated - 09/05/2024
Your Spaces
- RCNi Profile
- Steward Portal
- RCN Foundation
- RCN Library
- RCN Starting Out
Work & Venue
- RCNi Nursing Jobs
- Work for the RCN
- RCN Working with us
Further Info
- Manage Cookie Preferences
- Modern slavery statement
- Accessibility
- Press office
Connect with us:
© 2024 Royal College of Nursing
Important information about this website
From 1 July 2022, NHS Kirklees CCG will become part of NHS West Yorkshire Integrated Care Board . We will continue to work with health and care colleagues to improve outcomes for people in Kirklees and across West Yorkshire.
The changes mean that from 30 June, this website will be archived and will no longer be updated. A new website for the Kirklees Health and Care Partnership – http://www.kirkleeshcp.co.uk – will be launched on 1 July

Patient group directions and patient specific directions
Background and definitions.
The Human Medicines Regulations (2012) do not permit nurses, or other registered health care professionals (HCPs), who are not qualified prescribers, to administer or supply prescription only medicines (POMs) unless one of three types of instruction is in place:
- A signed prescription (must be signed prior to administration or supply to act as an instruction)
- Patient Specific Direction (PSD)
- Patient Group Direction (PGD)
Definition of a PGD
A Patient Group Direction is a legal (written) framework that allows the supply and/or administration of a specified medicine(s), by named, authorised, registered health professionals, to a pre-defined group of patients needing prophylaxis or treatment for a condition described in the PGD, without the need for a prescription or an instruction from a prescriber
- Most commonly used PGDs (for vaccinations and immunisations) are written by NHS England for use across many GP practices
- PGDs are legal documents which cannot be amended or deviated from
- PGDs cannot be used beyond their expiry date (unless an official extension letter has been received from CCG or NHSE)
- Expired PGDs should be removed from the master file and archived (not destroyed)
- All PGD documentation (including master authorised (signed) copies of PGDs, lists of authorised practitioners and patient supply/administration records and electronic records/agreements) must be kept for eight years for adults and for children until the child is 25 years old
- PGDs are not legally valid unless they have had the relevant organisational approval. Section 2 of the PHE PGD template requires a signature from the provider’s clinical governance lead, which is the site’s intention to ‘adopt’ the PGD and work under it
- This signature is in addition to the signature required to authorise named HCPs to work under the PGD, and is frequently missed
- A senior, responsible person from within the service should be identified to authorise named, registered HCPs (not including HCAs) to practice under the PGD e.g. GP, ANP
- HCPs must be trained, competent and authorised by the practice before operating under the PGD
Definition of a PSD
A Patient Specific Direction is an instruction (written or electronic instruction in patient notes) from a doctor, dentist, or non-medical prescriber for medicines to be supplied and/or administered to a named patient after the prescriber has assessed the patient on an individual basis
- Often used by suitably trained Health Care Assistants (HCAs) who are unable to work under PGDs as they are not a registered HCP e.g. for flu vaccinations
- Can be used by registered HCPs where a PGD is not available or appropriate e.g. B12 injections or Depo-Provera
- Can be a single written instruction or list of patients, signed by a prescriber
- Written PSDs should be scanned into the patients’ notes
- Can be electronic as long as it is placed in individual patient records by a prescriber. Ardens provide templates or practices may create their own
- Can be for a single event e.g. annual flu vaccination
- Can be for multiple events within a given timeframe e.g. B12 every 3 months for 12 months
NICE have provided a medicines practice guideline on PGDs , including developing, authorising, using and updating PGDs.
Further information for practices and PCNs on working with PGDs and PSDs and the legal requirements can be found on the Care Quality Commission’s (CQC) websit e
And on the Specialist Pharmacy Service website:
NHS England PGDs
PGDs to support GP practices with the national immunisation programme and NHS funded travel vaccinations (e.g. hepatitis A) that have been developed and signed off by NHS England. You can find information on the NHS England website .
These should be printed out, adopted by the practice and trained HCPs authorised to practice under them. Expired or superseded PGDs should be archived as above.
Advice for GP practices in implementing the national immunisation schedule
Full advice on immunisations can be found on the Government website .
Complete immunisation schedule .
PHE advice on Vaccination of Individuals with Uncertain or Incomplete Immunisation Status .
The following documents are being updated and will be published as soon as possible. In the meantime, you can find copies in our document archive . Please note that these documents may not be accessible if you are using assistive technology. If you need an accessible version, please contact [email protected] .
- Details of what legally needs to be in a PSD and recommendations for how to write a PSD for GP practices.
- Sample paper PSD for local amendment.
These documents allow some healthcare practitioners to supply or administer medicines without the need to get a prescription or patient specific direction.
For more information on Patient Group Directions visit the NHS England website .
You can find a leaflet that provides information for healthcare professionals on how to use PGDs on our document archive .

GP mythbuster 19: Patient Group Directions (PGDs)/Patient Specific Directions (PSDs)
Coronavirus (covid-19).
There have been no changes to the legislation relating to PGDs during the COVID-19 pandemic.
Organisations will need to consider local governance arrangements and perform local risk assessments if there is any divergence from their usual PGD related processes during a pandemic to ensure that PGD use remains within the legislation and that patient safety is protected.
COVID-19 Guidance has been provided by the Specialist Pharmacy Service for use of PGDs in pandemics (for example COVID-19) .
Staff who administer and/or supply prescription only medicines should have appropriate authorisation. Full details are listed in the information sources below. Providers should be aware of the requirements, but some of the key points are:
Patient Group Directions (PGDs)
PGDs are governed by the Human Medicines Regulations 2012 and later amendments. They allow specified health professionals to supply and/or administer medicine without a prescription or an instruction from a prescriber. The majority of clinical care should be provided on an individual basis using prescriptions or patient specific directions.
PGDs in commissioned NHS services
- Most PGDs are authorised before they are supplied to the practice for use in a commissioned service.
- These include PGDs authorised by the NHS England regional team to support the national immunisation programme.
- PGD is not valid until signed by a senior member of staff to adopt it for use by the provider.
Who can operate under a PGD?
Health professionals who may supply and/or administer medicines under a PGD are listed in the regulations . They include registered nurses, paramedics and pharmacists.
Examples of staff groups who cannot work under a PGD are:
- healthcare assistants
- nurse associates and
- physician associates.
The health professional who carries out the assessment under the PGD cannot delegate supply and/or administration to another member of staff.
Health professionals who will be using the PGD must be named and authorised before they use it to provide care. An appropriate member of staff, for example GP, practice manager or lead nurse should be responsible for authorising the health professionals in each organisation. Practitioners should keep a copy of their individual authorisation and have the current authorised PGD available for reference.
PGDs in Primary Care Networks (PCNs)
Where using patient group directions across primary care networks , each practice should adopt the PGD and authorise their staff to use it. Each practice is responsible for making sure their staff are trained, competent and complete necessary records.
There must be an agreement in place across the network to set out responsibilities and governance arrangements. Staff can then provide care under the PGD to patients of other practices covered by the agreement.
The provider must keep a record of all the health professionals authorised to practise under the PGD. Authorised health professionals must record an agreement to follow the PGD. They must provide assurances they are trained and competent to do so.
Electronic systems may be used to record authorisation, agreement and declarations of competence. If buttons or tick boxes are used it must be clear what the individual is confirming or signing up to. There must be a record of who has made the entry, the date and the time and an audit trail of any alterations.
Labelling and leaflets
- Medicines administered by the person operating under the PGD do not need to be labelled.
- Medicines do not need to be labelled if supplied under a PGD for immediate administration. For example, a flu vaccine nasal spray administered in the clinic to a child by their parent.
- Medicines supplied and taken away by the patient must be labelled in line with the regulations.
- Patient information leaflet must be supplied in every case, whether or not the medicine has to be labelled.
Developing PGDs for NHS or private services
A GP practice can develop their own PGDs to use for their NHS patients. There must be a formal agreement in place between the commissioner (the CCG or NHS England) and provider (the GP practice). This may be outlined in a service level agreement or contract specification.
GP practices and other providers can use PGDs in their private practice. For example, for the administration of travel vaccines such as yellow fever, rabies and Japanese B encephalitis. They can develop their own PGDs or buy authorised PGDs from an external organisation.
When developing their own PGDs providers should make sure they are aware of and follow the regulatory requirements for all areas of development, authorisation and use. Guidance is available in NICE MPG2 Patient group directions .
When buying a PGD the provider should make sure the organisation supplying the PGD has developed it in line with:
- regulations
- national guidance
- current clinical practice and
- is legally able to authorise the PGD.
Patient Specific Directions (PSDs)
A PSD is an instruction to supply and/or administer a medicine written and signed by the prescriber. It could be an electronic record made in the patient notes where it is identifiable to the prescriber.
A PSD can also be an instruction to administer a medicine to a list of patients. Each patient on the list must be individually assessed by that prescriber. The prescriber must have knowledge of the patient's health and be satisfied the medicine meets the individual needs of each patient on that list. For example, a healthcare assistant may be running an influenza immunisation clinic. The prescriber must review the patients attending the clinic and sign a list of those who they authorise to be immunised.
The PSD must include the:
- name(s) of patient(s) and/or other individual patient identifiers including age if a child
- name, form and strength of medicine
- route of administration
- date of treatment/number of doses/frequency/date treatment ends as applicable
- signature of prescriber.
During inspections we have seen cases where staff have mistakenly believed they were administering/supplying a medicine with the authority of a PSD. While it is not possible to list them all, the following are examples that do not meet the requirements of a PSD. They are not a legal authority for the administration or supply of medicines:
- a Patient Group Direction (PGD) template renamed a “PSD” and used to instruct healthcare staff.
- a generic instruction to be applied to any patient who may be seen by a healthcare professional or who has an appointment on any particular day. For example, an instruction to administer a flu vaccine to any patient who fits the criteria attending clinics on a specific day.
- a verbal instruction.
Responsibilities and accountabilities
- The prescriber is responsible for assessing the patient and making the decision to allow the supply or administration of the medicine.
- The prescriber must be satisfied that the person to whom administration is delegated has relevant qualifications, experience, knowledge and skills.
- A person supplying or administering medicine must be trained and competent.
- They must act in line with their level of competence and the directions of the prescriber.
What clinical governance arrangements should be in place?
In law, anyone whom the prescriber has:
- assessed as competent
- has the necessary knowledge and skills, and
- has been delegated the task may follow a PSD.
Some organisations may extend or limit those who are authorised to supply or administer medicines under a PSD. This must be documented in their local medicines policies and governance arrangements.
The practice has a duty of care to the patient and staff. They are responsible for making sure staff are properly trained and undertake only those responsibilities written in agreed job descriptions. If expecting non-regulated staff, for example healthcare assistants, to administer medicines, those delegating the duty must make sure these staff are competent to do so safely.
A locally approved procedure or guideline would support the safe administration of medicines by a suitably trained and competent healthcare professional.
What if a patient brings in prescribed medicines that have been dispensed for them elsewhere?
The practice may issue a prescription to a patient to have the medicine dispensed at a pharmacy or dispensary for administration at the practice. For example, the patient may obtain an injection such as vitamin B12 or Zoladex from a community pharmacy. The patient returns to the practice for it to be administered by the practice nurse. In these circumstances the responsibilities of the prescriber and the delegated member of staff administering the medicine are the same as for a PSD.
Further information
- Human Medicines Regulations 2012
- Patient Group Directions (Specialist Pharmacy Service)
- Questions about Patient Specific Directions (Specialist Pharmacy Service)
GP mythbusters
Snippet gp mythbusters rh.
Clearing up some common myths about our inspections of GP and out-of-hours services and sharing agreed guidance to best practice.
See all issues:
- GP mythbusters: listed by key question
- GP mythbusters: full list
- GP mythbusters: recently updated

Patient Specific Directions (PSDs) and Patient Group Directions (PGDs)
Page contents, patient specific directions (psds), patient group directions (pgds), frequently asked questions, guidance on developing a private pgd, psd for “group” administration e.g. flu vaccines, when no psd or pgd is needed – emergency drug exemptions.
The Medicines Act 1968 does not permit nurses who are not qualified prescribers to administer or supply prescription only medicines (POMs) unless one of three types of instruction are in place
- signed prescription
- signed Patient Specific Direction (PSD)
- Patient Group Direction (PGD)
If non-prescribing health care professionals are to administer a medicine on the instruction of a GP, the GP must be able to show that they have appropriate mechanisms in place to ensure that their practice meets statutory requirements. Since these mechanisms for supply and administration are statutory, the fact that a practice has followed them is mitigation to any ensuing liability.
A Patient Specific Direction is a written instruction from a doctor or dentist or other independent prescriber for a medicine to be supplied or administered to a named patient.
For example:
primary care: a prescription or simple written or electronic instruction in the patient’s notes (NB. This includes a letter from a consultant to the GP requesting that the patient commence on zoladex )
secondary care: instructions on a patient’s ward drug chart
PSDs do not limit those who can supply or administer the medicine. For example, a suitably trained health care assistant can do so, even though they cannot work under a PGD.
PSDs are also often used in relation to the administration of vaccinations for named patients as well as Depo-Provera, B12 and Zoladex.
Template PSD available for use if you wish
Back to Top
PGDs in Hampshire and IOW (Wessex)
PGDs in the South West (includes Dorset, BaNES, Swindon & Wiltshire)
The GPC’s guidance on Patient Group Directions (PGD) and Patient Specific Directions (PSD) in General Practice has been updated to clarify the rules surrounding private PGDs. Please click here to read the latest guidance: Patient Group Directions and Patient Specific Directions in General Practice January 2016
Guidance is also available on the Drugs and Prescribing page https://www.bma.org.uk/advice-and-support/gp-practices ?
https://www.cppe.ac.uk/e-learning/pgd/story_content/external_files/cppepgdtemplate.pdf
Patient Group Direction use in Primary Care Networks – https://www.sps.nhs.uk/articles/patient-group-direction-use-in-primary-care-networks/
The BMA/GPC advice changed in August 2010.
A Patient Group Direction is a written instruction for the supply and/or administration of a named licensed medicine for a defined clinical condition. PGDs allow a range of specified registered health care professionals to supply and/or administer a medicine directly to a patient with an identified clinical condition without them necessarily seeing a prescriber. The health care professional working within the PGD is responsible for assessing that the patient fits the criteria set out in the PGD. PGDs are intended to improve patient care by enabling registered health professionals other than doctors to supply and/or administer medicines to patients.Examples of where PGDs may be appropriate are services where assessment and treatment follows a clearly predictable pattern (eg immunisation, family planning).
In general practice they can be used to enable registered nurses to administer a prescription only medicine to a group of patients who fit the criteria specified in the PGD, for example, to administer vaccinations.
The following may supply or administer medicines under a patient group direction
- registered nurses
- health visitors
- optometrists
- pharmacists
- chiropodists
- radiographers
- orthoptists
- physiotherapists
- ambulance paramedics
- occupational therapists
- speech and language therapists
- prosthetists and orthotists
Note that they can only do so as named individuals.
Particulars to be included in a patient group direction
- The period the Direction shall have effect
- The description or class of POM (Prescription Only Medicine) to which the direction applies
- Whether there are any restrictions on the quantity of medicine which may be supplied on any one occasion, and if so, what restrictions
- the clinical situations which POMs of that description or class may be used to treat
- the clinical criteris under which a person shall be eligible for treatment
- whether any class of person is excluded from treatment under the Direction and, if so,what class of person
- whether there are circumstance in whigh further advice whould be sought from a doctor or dentist and,if so, what circumstances
- the pharmaceutical form or forms in which POMs of that description or class are to be administered
- the strength or maximum strength at which POMs of that description or class are to be administered
- the applicable dosage or maximum dosage
- the route of administration
- the frequency of administration
- any minimum or maximum period of administration applicable to prescription only medicines of that description or class
- whather there are any relevant warnings to note and, if so, what warnings
- whether there is any follow up action to be taken in any circumstances and, if so what action and in what circumstances
- Arrangements for referral for medical advice
- Details of the records to be kept of the supply, or the administration , of medicines under the Direction
Patient Group Direction (PGD) use in Primary Care Networks
Who in the practice needs to sign a PGD?
The authorising GP needs to sign a PGD naming the specific health care professionals who the PGD will apply to. In addition, the GPC and NMC recommend that the health care professional acting under the PGD must also sign the PGD.
Can electronic signatures be used on a PGD?
The Specialist Pharmacy Service (SPS) have a webpage giving details about electronic systems and PGDs. It says that “The MHRA have confirmed that electronic systems can be used to authorise a PGD”. You are recommended to read the guidance in full on the SPS website .
Can nurses who are not qualified prescribers administer or supply a prescription only medicine?
Yes. A GP can instruct a named practice nurse to supply or administer medicines to a patient. However medicines may only be administered by a practice nurse if one of three types of instruction are in place
- a signed prescription
- a signed Patient Specific Direction (PSD)
- a Patient Group Direction (PGD).
If one of these three options is not in place then the Medicines Act (1968) has been breached
Can a nurse independent prescriber administer a POM without a PSD or PGD in place?
Yes. Nurse independent prescribers do not require a PSD or PGD in order to administer a POM. Under the Medicines Act a nurse independent prescriber is able to administer any licensed medicine for any medical condition within their competence, including some controlled drugs for specified medical conditions.
What needs to be included in a PSD?
There is no set format for PSDs written into the legislation and you do not have it define an instruction as one. However a PSD must:
- state the name of the patient
- state the name and dose of the prescription only medicine to be administered
- show evidence to confirm that the patient has been considered as an individual.
A PSD may be a written or electronic instruction from the GP to the nurse in the patient record, relating to a specific individual patient.
Thus a verbal instruction or letters of invitation to a patient are not suitable.
A list of individually named patients to be treated with a named POM, signed by a doctor/prescriber would constitute a PSD in general practice, providing that each patient on the list has been considered individually by the doctor.
Practices must have protocols in place for their staff to follow to administer a POM using a PSD.
Can a nurse prescriber authorise a PSD?
Yes. Nurses may prescribe from the formulary linked to their recorded qualification. Nurse prescribers may issue a PSD and instruct another health care professional to administer the medicine.
When can PGDs be used in general practice?
In some circumstances, where assessment and treatment follows a clearly predictable pattern (for example where nurses are administering travel or childhood vaccinations) practices may find it beneficial to have an agreed PGD in place so that a GP does not have to give a specific instruction for each individual patient.
Nurses using PGDs must have been assessed as competent to use them and must comply with the standards set by their professional regulatory body the NMC (The Standards for Medicine Management1).
A PGD enables a nurse to supply and / or administer prescription-only medicines to patients using his / her own assessment of patient need, in accordance with the criteria set out in Schedule 7, Part I of Statutory Instrument 2000 No. 1917 – The Prescription Only Medicines (Human Use) Amendment Order 2000 (see below).
If there is no PGD in place then the nurse must have an individual instruction for that patient. This can be a PSD, or signed prescription.
Do PGDs apply to HCAs?
No. The Medicines Act does not allow HCAs to administer POMs under a PGD, as they are not included in the list of ‘authorised’ persons . An authorised person is one who is professionally regulated – HCAs therefore have to use a PSD or signed prescription as authority.
Can PGDs be used in General Practice to administer non-NHS treatment?
Under the Medicines Act GP practices are not permitted to use PGDs to enable nurses to administer treatment in NHS GP practices in non-NHS circumstances, for example providing private travel vaccinations such as Yellow Fever, Rabies, Meningitis etc.
Patient Specific Directions must be used in these circumstances unless they are independent prescribers. The National Travel Health Network and Centre (NaTHNaC) has proposed an amendment to the Medicines Act 1968 to the Department of Health to allow the use of PGDs in non-NHS circumstance, and the GPC supports this amendment.
Can PGDs be used for travel clinics?
PGDs are useful for NHS travel health services as in many practices these are delivered by practice nurses who have a special expertise in that field. However they can only be used for those treatments which are provided on the NHS and not for private treatment.
So where Hepatitis B vaccination can be given for travel and the patient is charged, a PGD cannot be used, but if it is given on the NHS then it can be administered under a PGD. This presents difficulties for some practices as many PCOs are trying to get practices to give Hepatitis B for travel as a private service which would make them ineligible for administration under a PGD and thus make the administration of the travel service more complex.
Can a GP sign off a PGD?
Not in the NHS. A PGD can only be signed off by a PCO when it applies to an NHS practice; if it is not signed off by the PCO, then it is not valid. This means that NHS practices are dependent on PCOs for the signing off of PGDs and can lead to PCOs using them to control or influence medicines use.
However GPs can be commissioned to provide clinical governance sign off for a PGD for a private practice or a private travel clinic (even though they cannot do so for their own NHS practice or clinic).
Can a PCO demand that a practice adopts a PGD for a particular POM?
No. The practice can determine how it wishes to organise the administration of medicines.
Can a PCO withdraw PGDs for certain medicines?
PCOs may try to do this in order to influence medicines use in the area. There is nothing in the legislation that states that PCOs have to develop PGDs, they merely have to authorise them.
If GP practices develop their own PGDs it would be difficult for a PCO to justify not approving it if all the conditions listed above have been met and there is a clinical need for the service. In this situation they would not be adhering to their obligations and duties to administer and provide health care to the public as set out in the NHS Act 2006.
Practices should, with LMC support, raise this with the PCO in writing justifying why a PGD is needed and clinical evidence of the need and quoting the PCO’s duties under the NHS Act and the amendment to the Prescription Only Medicines (Human Use) Order 1997 The Prescription Only Medicines (Human Use) Amendment Order 2000.
LMCs in their turn should support practices whose reasonable needs for a PGD are not being met by PCOs, especially where this is being done not on clinical grounds, but to manage prescribing. Please contact the GPC [email protected] for assistance this. If there are difficulties with the use of or production of PGDs then the practice can use patient specific directions where possible in order to continue providing the service though this may be a far less suitable and flexible method.
Can PCOs use PGDs as a performance management tool by putting unreasonable terms in them, for example excessive training requirements?
PGDs were intended to improve patient care by enabling registered healthcare professionals other than doctors to supply and / or administer medicines to patients. It is unreasonable and obstructive for PCOs to use PGDs to manage the way practices provide services. Only information listed above in Schedule 7, Part I of Statutory Instrument 2000 No. 1917 – The Prescription Only Medicines (Human Use) Amendment Order 2000 needs to be included in a PGD and if anything else is added by a PCO the practice should contact their LMC and raise these concerns before signing it.
Can PGDs be used to administer Botox?
No. The administration of medicines (such as Botox®, Vistabel® or Dysport®) to paralyse muscles which cause wrinkles requires assessment of individual patients’ suitability and (if the administration is to be delegated to a nurse or other person) patient specific directions. PGDs or general directions which would apply to any patient with an appointment on a particular day are not sufficient. In any case PGDs cannot be used to for private services in an NHS practice.
How long do you need to retain PGDs?
“PGD documentation includes master authorised (signed) copies of PGDs, lists of authorised practitioners and patient supply/administration records, including electronic records/agreements.
The same rules apply to PGD records as to all other patient records:
- For adults all PGD documentation in a patient’s clinical record must be kept for eight years.
- For children all PGD documentation in a patient’s clinical record must be kept until the child is 25 years old or for eight years after a child’s death.
- Where a PGD is for an implant in an adult then all PGD documentation in a patient’s clinical record must be kept for 10 years. For example this would apply to contraceptive and sexual health PGDs for contraceptive implants or drug eluting coils.
- Staff authorisation records should be kept for 8 years after the expiry date of the PGD if the PGD relates to adults only (10 years if relates to an implant) and for 25 years after the expiry date of the PGD if the PGD relates to children.
- The final authorised copy of the PGD should be kept for 8 years after the expiry date of the PGD if the PGD relates to adults only (10 years if relates to an implant) and for 25 years after the expiry date of the PGD if the PGD relates to children.
- The main content of a PGD (i.e. an unauthorised final copy), which contains no patient identifiable information or staff authorisation records, may be retained by an organisation for up to 20 years for purposes of business planning/continuity if there is reason to do so (i.e. reference for future PGDs).”
Retaining PGD documentation – SPS – Specialist Pharmacy Service – The first stop for professional medicines advice
https://www.nice.org.uk/guidance/mpg2
We do have to be mindful of the guidance around PGDs & PSDs and ensure we fulfill the recommendations.
What is a PSD?
“A written and authorised instruction to administer a medicine to a list of individually named patients where each patient on the list has been individually assessed by that prescriber. The prescriber must have adequate knowledge of the patient’s health and be satisfied that the medicine to be administered serves the individual needs of each patient on that list.
A written instruction applying to a group of patients where the patient/s are not individually identified i.e. a PSD could not state ‘All patients attending the practice’s ‘flu vaccine clinic on date dd/mm/yyyy’ but needs to be a list of all named patients due to attend the clinic who have been individually assessed by the prescriber as suitable for treatment and be signed and dated by a prescriber (this does not need to be completed for each entry but can be once for the entire list).” https://www.sps.nhs.uk/articles/questions-about-patient-specific-directions-psd/
“Group PSD”
This is a link to a Group PSD adapted from one written by Diane Coulthard who is an excellent trainer in vaccinations and immunisations. You could adapt this in your practice to allow HCAs and staff not directly employed by the practice and not non-medical prescribers e.g. paramedics/pharmacists to administer flu vaccines.
In addition, we would recommend that the following needs to be put in place;
The PSD must clearly identify which flu vaccine is to be administered under this specific PSD i.e. Quadrivalent or Trivalent as there should be a separate PSD for each vaccine. This may require practices organising separate clinics for administration of each vaccine.
The person signing the PSD must be satisfied that they are not aware of any contraindications to the patients on the list receiving the stated vaccine, as they are taking responsibility for making the clinical decision.
The person signing the PSD must be confident that they are singing that the person administering the vaccine is competent, has received training in administering the flu vaccines, is aware of the cold chain policy, clinically supervised and has attended annual up to date training around basic life support, management of anaphylaxis and use of the defibrillator.
There should be a record in the patients notes that the vaccine has been administered via a PSD. You would benefit from speaking to your IT person to add in a short cut key or read code.
The printed list of patients under the PSD should be retained for at least 2 years and preferably stored electronically.
As with all vaccines the patients name, DOB, type of vaccine, expiry date, vaccine code, method of immunisation and site of injection should be recorded in the patients notes together with patients consent to administration.
Hampshire & Isle of Wight Patient Group Direction Downloads – Standalone PGDs
PGDs in the South West
HCAs & Immunisations/PSDs
The following is taken form the RCN document Health Care Support Workers Administering Inactivated Influenza, Shingles and Pneumococcal Vaccines for Adults and Live Attenuated Influenza Vaccine (LAIV) for Children
Questions about Patient Specific Directions (SPS, 2018) states the following:-
- The prescriber is responsible for assessment of the patient and the decision to authorise the supply/administration of the medicine(s) in question.
- The prescriber has a duty of care and is professionally and legally accountable for the care they provide.
- The prescriber must be satisfied that the person to whom the administration is delegated has the qualifications, experience, knowledge and skills to provide the care or treatment involved.
This is also clear within the GMC’s (2014) Good medical practice guidance and the NMC’s (2018) The Code for nurses and midwives.
HCSWs must not be placed in a position where they need to make standalone clinical judgment calls in relation to vaccine administration. The HCSW needs to be able to promptly liaise and discuss issues with a registered health care professional who is available on site (whether they are in a primary care, school or hospital setting). For practical and general administration issues, this can be any registered health care professional but for medicines and prescribing clarification the registered prescriber needs to be available.
All registered professionals must adhere to their codes of conduct, standards of practice and delegation principles (NMC, 2018; GMC, 2014; HCPC, 2016; GPhC, 2017).
The following list of medicines for use by parenteral administration, are exempt from PGDs, prescriptions or PSDs when administered for the purpose of saving life in an emergency:
Doses are not specified in the legislation
- Adrenaline 1:1000 up to 1mg for intramuscular use in anaphylaxis
- Atropine sulphate and obidoxime chloride injection
- Atropine sulphate and pralidoxime chloride injection
- Atropine sulphate injection
- Atropine sulphate, pralidoxime mesilate and avizafone injection
- Chlorphenamine injection
- Dicobalt edetate injection
- Glucagon injection
- Glucose injection
- Hydrocortisone injection
- Naloxone hydrochloride
- Pralidoxime chloride injection
- Pralidoxime mesilate injection
- Promethazine hydrochloride injection
- Snake venom antiserum
- Sodium nitrate injection
- Sodium thiosulphate injection
- Sterile pralidoxime
Reference: http://www.legislation.gov.uk/ukpga/1968/67
Please login to bookmark

What is a Patient Group Direction (PGD)?
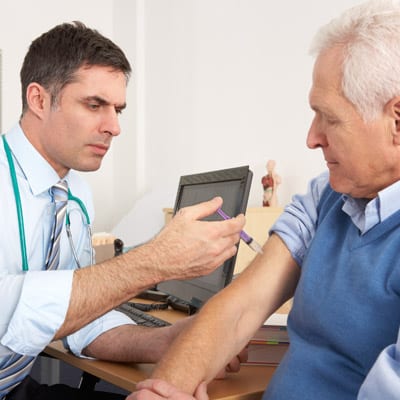
With the flu vaccination season almost upon us, I thought I would highlight the need for – and use – of PGDs. PGDs are the legal mechanism by which a prescription only medicine (POM) can be supplied or administered to a patient for whom no individual prescription exists. All vaccines come under the legal category of POMs. PGDs were introduced through legislation in 2000 and are written agreements for the supply and administration of medicines to groups of patients who may not be identified before presentation for treatment.
What is the difference between a PGD and a PSD?
PGDs can be used for patient groups where general requirements are sufficiently consistent to be provided for by such a non-specific direction e.g. childhood immunisations. A Patient Specific Direction (PSD) is the traditional written instruction, signed by a doctor, dentist, or non-medical prescriber for medicines to be supplied and/or administered to a named patient after the prescriber has assessed the patient on an individual basis. Where a PSD exists there is no need for a PGD. Practices are able to develop their own PGDs if they need to but they must have an agreement with an authorising body such as NHS England or the local Clinical Commissioning Group (CCG).
Who can use PGDs?
We’ve received a few PGDs lately, including the administration of Men C for children aged 2 months to 10 years, and the new Men ACWY vaccine. PGDs can only be provided for specific health professionals and generally includes nurses, midwives, pharmacists, ambulance paramedics, occupational therapists, and dental therapists. Whoever is responsible under the PGD for the supply and administration of medicines must be named on the PGD and this responsibility cannot be passed to others. Implementation of the PGD must be outlined in the specification and only trained and competent staff can administer medicines and vaccines under the PGD.
What should be in a PGD?
Besides the name of the service provider and individuals to whom the PGD applies, other information which should be contained in PGD documentation includes:
- The valid from and expiry date of the PGD
- The medicines to which the PGD applies
- The clinical condition or situation to which the PGD applies
- The criteria for exclusion under the PGD e.g. patient’s aged and medical history
- The description of treatment, including the name, strength and formulation
- The dose and frequency of administration
- The disposal of the medicine
- Any drug interactions, and the management of adverse reactions
Further information about PGDs can be sought from NICE and the RCN .
Alison Lowerson – QCS Expert GP Practice Manager Contributor
Share:

📢 Introducing Quality Centre: Your go to product for audits and digital mock inspections!
Get FREE and instant access to the UK’s leading compliance system with over 340 policies and procedures
Cookies on the NHS England website
We’ve put some small files called cookies on your device to make our site work.
We’d also like to use analytics cookies. These send information about how our site is used to a service called Google Analytics. We use this information to improve our site.
Let us know if this is OK. We’ll use a cookie to save your choice. You can read more about our cookies before you choose.
Change my preferences I'm OK with analytics cookies
Patient Group Directions (PGD)
Patient Group Directions (PGD) for the supply and administration of vaccinations as part of the national immunisation schedule.
The legal definition of a PGD is “a written instruction for the supply and/or administration of a licensed medicine (or medicines) in an identified clinical situation, signed by a doctor or dentist and a pharmacist”. It applies to groups of patients who may not be individually identified before presenting for treatment.
NHS England/UKHSA has produced a suite of PGDs for Practices that have been commissioned by NHS England to deliver immunisations as set out in the Section 7a agreement .
The PGDs cover the authorisation of staff, documentation, audit requirements and general guidance on best practice required to safely administer vaccines.
Please note: It is the clinician’s responsibility to ensure that the PGDs they are using are up to date. If a PGD has expired and it has not been updated, these immunisations should be administered under a Patient Specific Direction (PSD) instead.
The following PGDs are for use by Practice Nurses in the East of England only.
The team provide immunisation support to health professionals. They can be contacted via the following email addresses:
- For East Anglia: [email protected]
- For Essex: [email protected]
- For Herts and BLMK (Bedfordshire, Luton and Milton Keynes): [email protected]
COVID-19 PGDs are available via UKHSA
PGD List and Expiry Dates January 2024
Be advised there are now three PGD extensions (Zostavax and Hep A/Typhoid and PCV at risk). The information can be found here
******************PLEASE ENSURE GUIDANCE IS ACCESSED THROUGH THE LINKS PROVIDED. ANY ITEMS PRINTED MAY QUICKLY BECOME OUT OF DATE********************
Diphtheria, Tetanus, Acellular Pertussis and Inactivated Poliomyelitis Vaccine Patient Group Direction (PGD)
This PGD is for the administration of diphtheria, tetanus, acellular pertussis and inactivated poliomyelitis vaccine (dTaP/IPV) to individuals from 3 years 4 months to under 10 years of age, in accordance with the national immunisation programme in England, or for the management of cases and contacts of diphtheria, tetanus, pertussis or poliomyelitis from 3 years of age.
Diphtheria, tetanus, acellular pertussis, inactivated poliomyelitis, Haemophilus influenzae type b and hepatitis B vaccine (DTaP/IPV/Hib/HepB) PGD
This PGD is for the administration of diphtheria, tetanus, acellular pertussis, inactivated poliomyelitis, Haemophilus influenzae type b and hepatitis B (DTaP/IPV/Hib/HepB) vaccine to individuals from 6 weeks (routinely 8 weeks) to under 10 years of age in accordance with the national immunisation programme or for the management of cases and contacts identified in an outbreak of polio in accordance with the National polio guidelines: Local and regional services and recommendations from the local health protection team.
Haemophilus influenzae type b and meningococcal C conjugate vaccine (Hib/MenC) Patient Group Direction (PGD)
This PGD is for the administration of Haemophilus influenzae type b and meningococcal C conjugate vaccine (Hib/MenC) to individuals from their first birthday to under 10 years of age in accordance with the national immunisation programme; and to individuals of any age for the prevention of secondary cases of meningococcal group C (MenC) disease.
Hepatitis B vaccine Patient Group Direction (PGD)
This PGD is for the administration of Hepatitis B recombinant DNA (rDNA) vaccine (adsorbed) to individuals considered at increased risk of exposure to hepatitis B virus, at increased risk of complications of hepatitis B disease, or post potential exposure to hepatitis B virus.
Hepatitis B vaccine Renal Patient Group Direction (PGD)
This PGD is for the administration of Hepatitis B recombinant DNA (rDNA) vaccine (adsorbed) to individuals who are 15 years of age or over and are on haemodialysis, a renal transplantation programme or have chronic renal failure that is likely to require haemodialysis or transplant.
HPV Vaccine PGD GOV-14792
This PGD is for the administration of human papillomavirus (HPV) vaccine to individuals from 12 years of age or from school year 8 and aged less than 25 years in accordance with the national immunisation programme.
Meningococcal group A, C, W and Y (MenACWY) conjugate vaccine PGD
This PGD is for the administration of meningococcal groups A, C, W and Y conjugate vaccine (MenACWY) to individuals eligible for the national routine MenACWY vaccination programme or identified as a contact of a case of invasive meningococcal disease, in accordance with the Green Book and Guidance for Public Health Management of Meningococcal Disease in the UK.
Meningococcal Group A, C, W, and Y Conjugate Vaccine for Risk Groups Patient Group Direction (PGD)
This PGD is for the administration of meningococcal group A, C, W, and Y conjugate vaccine (MenACWY) to individuals with an underlying medical condition which puts them at increased risk from Neisseria meningitidis.
Meningococcal Group B Vaccine Patient Group Direction (PGD)
This PGD is for the administration of meningococcal group B vaccine (rDNA, component, adsorbed) (4CMenB) to individuals from 8 weeks of age eligible for the national routine immunisation programme and to individuals for the prevention of secondary cases of meningococcal group B disease.
Meningococcal Group B Vaccine Risk Groups Patient Group Direction (PGD)
This PGD is for the administration of meningococcal group B vaccine (rDNA, component, adsorbed) (4CMenB) to individuals, from 2 years of age, with an underlying medical condition which puts them at increased risk from Neisseria meningitidis group B.
MMR Measles, mumps and rubella Patient Group Direction (PGD)
This PGD is for the administration of measles, mumps and rubella (MMR) vaccine to individuals from one year of age for routine immunisation, or from 6 months of age if early protection is required, in accordance with the national immunisation programme and the National measles guidelines.
Pneumococcal polysaccharide conjugate vaccine (adsorbed) Patient Group Direction (PGD)
This PGD is for the administration of pneumococcal polysaccharide conjugate vaccine (13-valent or 15-valent, adsorbed) (PCV) to individuals from 12 weeks to under 2 years of age in accordance with the national immunisation programme for active immunisation against pneumococcal disease and to individuals from 6 weeks of age recommended PCV13 or PCV15 in response to an outbreak of pneumococcal disease.
Pneumococcal polysaccharide conjugate vaccine (13-valent, adsorbed) Risk Groups Patient Group Direction (PGD)
This PGD is for the administration of pneumococcal polysaccharide conjugate vaccine (13-valent, adsorbed) (PCV13) to individuals from 6 weeks of age with an underlying medical condition which puts them at increased risk from pneumococcal disease.

Pneumococcal polysaccharide conjugate vaccine (13-valent, adsorbed) Risk Groups Patient Group Direction (PGD) **EXPIRY DATE EXTENSION TO PGD NOW VALID UNTIL 28 FEB 2025**
This PGD extension is for the administration of pneumococcal polysaccharide conjugate vaccine (13 -valent, absorbed) (PCV13) to individuals from 6 weeks of age with an underlying medical condition which puts them at increased risk from pneumococcal disease.
Pertussis Vaccine Patient Group Direction (PGD)
This PGD is for the administration of low dose diphtheria, tetanus, acellular pertussis and inactivated poliomyelitis vaccine (dTaP/IPV) to pregnant women from week 16 of pregnancy, in accordance with the national immunisation programme and to pertussis contacts aged 10 years and over in accordance with Guidelines for the Public Health Management of Pertussis in England and Guidelines for the Public Health Management of Pertussis Incidents in Healthcare Settings.
Pneumococcal polysaccharide vaccine (PPV23) Patient Group Direction (PGD)
This PGD is for the administration of 23-valent pneumococcal polysaccharide vaccine (PPV23) to individuals from 65 years of age and individuals from 2 years of age in a clinical risk group in accordance with the national immunisation programme for active immunisation against pneumococcal disease and UK guidelines for the public health management of clusters of severe pneumococcal disease in closed settings.
Rotavirus vaccine Patient Group Direction (PGD)
This PGD is for the administration of rotavirus vaccine (live) to infants aged 6 weeks to 23 weeks and 6 days for active immunisation against rotavirus.
Shingrix® Herpes Zoster Vaccine Patient Group Direction
This PGD is for the administration of Shingrix® Herpes Zoster Vaccine (recombinant, adjuvanted), for the prevention of herpes zoster (‘zoster’ or shingles) and herpes zoster-related post-herpetic neuralgia (PHN), to individuals who are eligible for the national shingles immunisation programme.
Low-dose diphtheria, tetanus and inactivated poliomyelitis vaccine (Td/IPV) Patient Group Direction (PGD)
This PGD is for the administration of low-dose diphtheria, tetanus and inactivated poliomyelitis vaccine (Td/IPV) to individuals from 10 years of age, in accordance with the national immunisation programme in England, for travel, or for the management of cases and contacts of diphtheria, tetanus or poliomyelitis.
Varicella vaccine (live) Patient Group Direction (PGD)
This PGD is for the administration of varicella vaccine (live) to individuals identified for pre exposure prophylaxis, and where chickenpox is co-circulating with Group A Streptococcus (GAS) infections, for post exposure prophylaxis in non immune children, from 9 months of age and adults in accordance with national guidelines.
Zostavax® vaccine Patient Group Direction (PGD)
This PGD is for the administration of Zostavax®, shingles (herpes zoster, live) vaccine, to individuals who are eligible for the national shingles immunisation programme for the prevention of herpes zoster (‘zoster’ or shingles) and herpes zoster-related post-herpetic neuralgia (PHN).
PGD 13_Zostavax v11.00 (GOV-15000), expiry date extended to 31 OCTOBER 2024
This PGD is extended and valid until 31 October 2024, reflecting the longest-dated shelf life of centrally supplied stock of Zostavax®, following its phasing out from the shingles vaccination programme.
Typhoid Vi Polysaccharide Vaccine Patient Group Direction (PGD)
This PGD is for the administration of typhoid Vi polysaccharide vaccine to overseas travellers at risk of exposure to Salmonella enterica serovar typhi (S. typhi) in accordance with recommendations from the National Travel Health Network and Centre (NaTHNaC).
HepA/B Vaccine Patient Group Direction (PGD)
This PGD is for the administration of hepatitis A virus (inactivated) and hepatitis B recombinant DNA (rDNA) (HepA/B) vaccine (adsorbed) to individuals requiring protection against hepatitis A and hepatitis B virus in accordance with national recommendations.
Combined Hepatitis A Virus (Inactivated) and Typhoid Polysaccharide Vaccine Patient Group Direction (PGD)
This PGD is for the administration of combined hepatitis A virus (inactivated) and typhoid polysaccharide vaccine (HepA/Typhoid) to individuals considered at risk of exposure to Salmonella enterica serovar typhi, (S. typhi) and hepatitis A virus in accordance with recommendations from the National Travel Health Network and Centre (NaTHNaC).
PGD 23_Hepatitis A and typhoid v3.00 (GOV-11415), expiry date extended to 31 MAY 2024
This PGD is extended and valid until 31 May 2024, reflecting the longest-dated stock of ViATIM®, following its withdrawal from the UK market in Autumn 2022.
Hepatitis A Vaccine Patient Group Direction (PGD)
This PGD is for the administration of Hepatitis A virus (inactivated) vaccine (adsorbed), to individuals considered at high risk of exposure to hepatitis A or post exposure to hepatitis A virus in accordance with national recommendations.
Cookies on GOV.UK
We use some essential cookies to make this website work.
We’d like to set additional cookies to understand how you use GOV.UK, remember your settings and improve government services.
We also use cookies set by other sites to help us deliver content from their services.
You have accepted additional cookies. You can change your cookie settings at any time.
You have rejected additional cookies. You can change your cookie settings at any time.
- Health and social care
- Medicines, medical devices
Proposal for the use of patient group directions by pharmacy technicians
- Department of Health & Social Care
Updated 28 March 2024
Applies to England, Scotland and Wales

© Crown copyright 2024
This publication is licensed under the terms of the Open Government Licence v3.0 except where otherwise stated. To view this licence, visit nationalarchives.gov.uk/doc/open-government-licence/version/3 or write to the Information Policy Team, The National Archives, Kew, London TW9 4DU, or email: [email protected] .
Where we have identified any third party copyright information you will need to obtain permission from the copyright holders concerned.
This publication is available at https://www.gov.uk/government/consultations/proposal-for-the-use-of-patient-group-directions-by-pharmacy-technicians/proposal-for-the-use-of-patient-group-directions-by-pharmacy-technicians
Introduction
This consultation seeks views on the proposal to enable registered pharmacy technicians to supply and administer medicines under a patient group direction ( PGD ).
It is the ambition of NHS systems across the United Kingdom to maximise the use of the skill mix in pharmacy teams, enabling them to meet more of the health needs of their local populations. By utilising the skills of the whole pharmacy team, pharmacists in community pharmacy will be enabled to deliver more patient-facing clinical services, improving access to care for patients and releasing capacity in the wider NHS. Across other clinical settings this proposal will enable registered pharmacy technicians to maximise the contribution they make within multi-professional teams through more effective use of their unique skills and expertise.
This proposal is supported by all 4 nations across the UK where the future ambitions for the pharmacy technician profession are addressed in the documents below:
- in England: supports the delivery of the NHS Long Term Plan , the NHS Long Term Workforce Plan and the Delivery plan for recovering access to primary care
- in Scotland: supports the future vision for pharmacy in Pharmacy 2030: a professional vision
- in Wales: supports the achievement of ambitions set out in Pharmacy: delivering a healthier Wales and A new prescription
- in Northern Ireland: supports the commitment to develop the pharmacy technician profession in the Pharmacy workforce review 2020 and Introduction of statutory regulation of the pharmacy technician
A PGD is a written instruction that permits listed healthcare professionals to supply or administer medicines to a pre-defined group of patients. The aim of this proposal is to make it easier for patients to get the medicines they need when they need them, while maintaining public safety. This will avoid the requirement for patients to see additional healthcare professionals just to receive medicines, where it is safe and appropriate to do so, thereby facilitating timely access to medicines, improving patient care and patient experience.
The Secretary of State for Health and Social Care, in relation to England and Wales and Scotland, in conjunction with the Department of Health in Northern Ireland in relation to Northern Ireland (pursuant to Section 45(1) of the Medicines and Medical Devices Act 2021 ), is seeking views on the proposal to amend the Human Medicines Regulations 2012 ( HMRs ) to allow registered pharmacy technicians to supply and administer medicines under a PGD .
The amendment will be implemented by a statutory instrument (SI) under enabling powers in the Medicines and Medical Devices Act 2021 ( MMD Act). The proposed changes would enable registered pharmacy technicians to use PGDs across England, Wales and Scotland in any setting including the NHS, independent and voluntary sectors. However, these powers do not mean that organisations are required to implement the use of PGDs by registered pharmacy technicians. PGDs should only be used where there is clear benefit for patient care without compromising patient safety and where there are clear governance arrangements and accountability.
Pharmacy technicians in Northern Ireland are not a registered healthcare profession so amendments to the HMRs cannot currently allow pharmacy technicians in Northern Ireland to use PGDs . However, once pharmacy technicians in Northern Ireland become a registered healthcare profession, a further amendment to the HMRs may be made so they can also use PGDs .
Proposal to change the Human Medicines Regulations 2012 ( HMRs ) for registered pharmacy technicians
Patient group directions ( pgds ).
A PGD is a written instruction that allows healthcare professionals specified within the HMRs to supply and/or administer a medicine directly to a group of patients with an identified clinical condition. PGDs are not a form of prescribing.
A PGD allows the supply and administration of named medicines in an identified clinical situation, without the need for an appropriate prescriber under the HMRs to provide an individual written prescription. A PGD is a legal mechanism for the administration and/or supply of a medicine. The healthcare professional working within the PGD is responsible for assessing that the patient fits the criteria set out in the PGD and should or should not be supplied or have administered the medicine concerned. The supply and/or administration of medicines under a PGD cannot be delegated - the whole episode of care must be undertaken by the healthcare professional operating under the PGD . A separate PGD is recommended for each different medicine to be supplied or administered.
PGDs are developed by multi-professional groups with extensive expertise, requiring a significant amount of time and resource to develop and authorise. Once implemented, PGDs are subject to ongoing monitoring. The governance involved in the consideration, development, authorisation and maintenance of PGDs ensures the safe and effective supply and administration of medicines by a designated healthcare professional. As set out in schedule 16 of the HMRs , the following list of registered healthcare professionals are permitted to supply and administer medicines under a PGD :
- pharmacists
- registered chiropodists and podiatrists
- registered dental hygienist
- registered dental therapist
- registered dietitians
- registered midwives
- registered nurses
- registered occupational therapists
- registered optometrists
- registered orthoptists
- registered orthotists and prosthetists
- registered paramedics
- registered physiotherapists
- registered radiographers
- registered speech and language therapists
While these healthcare professionals are eligible to use PGDs , it is for local organisations to agree the appropriateness for their use within a clinical service using the national guidelines and local governance to inform the decision.
There are no current plans to amend the Misuse of Drugs Regulations 2001 to enable registered pharmacy technicians to supply and/or administer controlled drugs in any of the 5 schedules under a PGD .
Use of PGDs by private practitioners
As General Pharmaceutical Council ( GPhC ) regulated healthcare professionals, pharmacy technicians working in private practice are governed and regulated by the same standards as those working in the NHS, and the standard of care expected is the same. Should PGDs be permitted within the clinical setting, PGDs should be written, authorised and implemented in line with all the relevant national and local governance requirements, and developed according to National Institute of Clinical Excellence ( NICE ) guidance, Medicines practice guidance (MPG2) . Employers outside the NHS have the same roles and responsibilities as those within the NHS and must implement the same standard of local governance arrangements related to the safe storage, supply and administration of medicines.
In addition, their practice or clinic must also be registered and regulated by one of the following, depending on the location of the practice:
- in England, the Care Quality Commission (CQC) - the independent regulator of health and adult social care service providers in England or the GPhC if it is a registered pharmacy
- in Wales, Healthcare Inspectorate Wales - the independent inspectorate and regulator of healthcare in Wales
- in Northern Ireland, the Regulation and Quality Improvement Authority - responsible for inspecting the availability and quality of health and social care services
- in Scotland, Healthcare Improvement Scotland - responsible for regulating independent healthcare services
Benefits of registered pharmacy technicians being able to supply and administer under PGDs
The only mechanism by which registered pharmacy technicians can currently supply and administer medicines is where they are authorised to do so by a patient specific direction ( PSD ). A PSD is a written instruction to supply or administer a medicine to a named patient who has been assessed on an individual basis by the authorised prescriber who then prescribes the medicine. The PSD enables a pharmacy technician to administer or supply the medicine to the patient.
This does not fully utilise the skills and knowledge of registered pharmacy technicians who could, as registered healthcare professionals, use their education and training to supply and administer medicines safely under a PGD . If PGDs were in place, registered pharmacy technicians could administer specific medicines under an appropriate PGD without requiring the intervention of trained prescribers. This would enable pharmacy technicians to take responsibility for their decisions to administer and supply medicines in accordance with the written PGD . The PGD provides a clear scope of practice with specific education and governance requirements defined by appropriate clinical governance assurance processes.
The use of PGDs for the supply and/or administration of medicines can bring benefits to patients, commissioners and providers. Registered pharmacy technicians can use their medicines expertise to help make every contact count and reduce further health interventions. The proposed use of PGDs will enable patients to access the medicines and services they require in a timely and effective manner, avoiding the risks associated with delayed care, and improving patient outcomes. With the continuing expansion of more than 4,500 registered pharmacy technicians working in primary care, the opportunities for patient-centred service redesign are critical to enable improved access to healthcare, address health inequalities and reduce burden on general practice.
All 4 nations of the UK want to further integrate community pharmacy into the NHS. By better utilising the clinical skills of pharmacy teams, community pharmacies will be able to provide more NHS clinical services closer to where people live and become the first contact for managing minor self-limiting illnesses. Within community pharmacy, this proposal will enable registered pharmacy technicians to supply and administer certain medicines directly under a PGD , without the requirement to obtain a PSD from an independent prescribing pharmacist.
This is pertinent as initial education and training reforms will see pharmacists become independent prescribers from the point of registration from 2026 onwards. As part of this reform, registered pharmacy technicians will be required to capitalise on their registered status and post-registration education to deliver a broader range of tasks. This will enable independent prescribing pharmacists to deliver more clinical orientated services, particularly in community pharmacy and general practice settings.
Taken together, independent prescribing pharmacists and the use of PGDs by registered pharmacy technicians could increase the capacity for prescribing, supply and administration of medicines. Within community pharmacies this will provide patients with access to a wider range of clinical services delivered by healthcare professionals with the right skills at the right time, supporting improved patient outcomes. It could also reduce demand in other parts of the healthcare system.
Overall, this proposal increases access to medicines for patients by improving convenience and efficiency of service delivery, and by maximising appropriate use of professionals in the team.
It is for commissioners (national and local) to monitor the use of PGDs , including examples of how they contribute to wider ambitions, such as freeing up other healthcare professionals’ time or reducing the pressure elsewhere in the NHS.
Use in clinical practice (scenarios)
The examples below demonstrate the breadth and contributions the profession could support across healthcare sectors to support expansion of service accessibility for patients.
Registered pharmacy technicians administering vaccines
Pharmacy technicians have responded rapidly and professionally to the pandemic and all its challenges. Through late 2020 and early 2021 there was rapid mobilisation of the profession to support the distribution, preparation and administration of the COVID-19 vaccine on NHS sites and other centres.
The experience, skills and knowledge of pharmacy technicians has contributed to the success of the vaccination programme - from receipt, stock management and distribution of the vaccine, to support with preparation of the vaccine prior to administration.
The current legal and governance framework does not allow registered pharmacy technicians to administer vaccines where vaccination centres choose to operate their vaccination programme under a PGD .
Pharmacy technicians have become an integral part of the COVID-19 vaccination roll out and delivery. Pharmacy technicians have been able to administer vaccines where the choice of legal mechanism to support service has been via PSD or national protocol.
There is working experience and evidence of successful implementation of pharmacy technician skills across all parts of the patient’s vaccination journey, from receipt of vaccine to administration. The success of the national COVID-19 vaccination roll out and delivery relies on the ability to operate effectively and with ‘lean’ processes that maximise the skill sets available by the staff engaged in providing the service.
The current model does not allow registered pharmacy technicians to fully participate, as the legal framework excludes them from certain parts of the process (for example, patient consent). This leads to fragmentation in service provision that could be addressed using a PGD that allows registered pharmacy technicians who complete specific PGD training, and are deemed competent, to be involved in the whole process.
Including pharmacy technicians as registered healthcare professionals able to supply and administer medicines under a PGD will result in longer-term benefits for patients. There are clear benefits to be realised from a service provision model that uses a more holistic approach to the patient vaccination journey, both in terms of patient safety and service effectiveness.
The scale of vaccination programmes for both COVID-19 and influenza means that pharmacy technicians have the potential to contribute more to other immunisation programmes by enabling them to administer vaccines under PGDs . They are well positioned and have demonstrated they have the required skill set and knowledge to support this safely and effectively.
Registered pharmacy technicians administering emergency contraception ( EC )
The most recent UK estimates from the National Survey of Sexual Attitudes and Lifestyles (NATSAL) were that 45% of pregnancies were unplanned or ambivalent (Lancet, 2013). This leads to high costs within the NHS, with direct medical costs of £193,200,000 in 2010. It is clear to see the potential cost savings of a programme of preconception care that simultaneously seeks to prevent unwanted pregnancies while improving the planning and preparation of those that are desired. There were 817,515 conceptions in 2020 to women aged 15 to 44 years in England and Wales.
Registered pharmacy technicians in community pharmacy are well positioned to supply emergency contraception ( EC ). Along with EC PGD competency training, the underpinning knowledge gained in human physiology, pharmacology of medicines and patient consultation skills provides a sound basis to enable appropriate assessment of the presenting patient in terms of:
- suitability and eligibility for a supply (inclusion criteria, concomitant medication and medicines interactions)
- ability to signpost patients to appropriate services, should they not be eligible
- advice in relation to administration, side effects and risks should the patient decline treatment after counselling
The supply associated with the PGD is defined and there is a standard dose requiring no adjustment or calculation. Including registered pharmacy technicians in EC supply under a PGD gives pharmacies the ability to offer presenting patients a wider range of pharmacy professionals with which to discuss their treatment. This may be preferable in a sensitive situation and could expand the pharmacies capacity to provide a broader range of services.
Registered pharmacy technicians administering oral contraception (OC)
Several contraception services have been commissioned across the UK. For example, in April 2023, the NHS Pharmacy Contraception Service was introduced in England as an advanced service under the Community Pharmacy Contractual Framework (CPCF). The service provides ongoing oral contraception for women, initiated in primary care or sexual health clinics (or equivalent) and is undertaken using PGDs . Similarly, bridging contraception (desogestrel) administered via PGD was introduced in Scotland in November 2021 under the Public Health Service element of the Scottish Contract.
Currently, these services are provided by a pharmacist, although there is scope for registered pharmacy technicians to deliver them if they can demonstrate evidence of competence in the clinical skills and knowledge required to provide the service. This will free up pharmacists’ time, which could be used to focus their clinical expertise on treating more complex cases within community pharmacy.
Registered pharmacy technicians in pre-op clinic
The pharmacy technician’s role in pre-op clinic includes medicines reconciliation, medication supply, patient counselling and discharge facilitation, often in patients categorised as ‘low risk’ on specific elective pathways. As part of the multi-professional team pharmacy technicians often:
- complete the patient assessment prior to surgery
- take and confirm medication history
- transcribe inpatient prescription charts ready for inpatient stay
- provide advice and information about medication both pre-op and post-op, including what to stop and start, to minimise risks and optimise outcomes
In all circumstances the pharmacy technician can refer to a pharmacist or clinician. This allows pre-op clinical pharmacists to target their resources towards the management of more complex and/or high-risk patients, and for nursing time to be released for other duties or roles in the pre-op clinic. To further maximise the skill mix and resource in the multi-professional team and to enhance patient safety and experience, registered pharmacy technicians who complete specific PGD training and are deemed competent, could supply patients with pre-operative bowel cleansing preparations (prior to colorectal surgery) or prescription only medication for pre-op Methicillin-resistant Staphylococcus aureus (MRSA) decolonisation.
The pharmacy technician’s underpinning knowledge, skills and competency support their role in:
- assessing patient suitability and eligibility (including interpretation of patient results and medication history)
- assessing consent
- providing verbal and written advice and information to ensure appropriate administration by the patient
- documentation in patient’s record
- referral to clinicians, where appropriate
Governance and patient safety
As with any of the professions authorised to use PGDs , registered pharmacy technicians will be required to demonstrate they are competent to do so.
The governance involved in developing a PGD ensures there is clear accountability, delegation, monitoring and a structured work programme for reviewing, updating and re-authorising PGDs . Together with the governance set by the professional regulator (see below), these measures provide assurance to patients and healthcare professional colleagues that registered pharmacy technicians can supply and administer medicines using a PGD safely and appropriately.
The role of a pharmacy technician
Pharmacy technicians are involved in the procurement, storage, supply, preparation, administration and education of medicines and medicinal products. They work as part of multi-professional teams and provide medicines optimisation services. Place-based training of pharmacy technicians provides exposure to the clinical setting in which they will be delivering medicines optimisation services. These clinical settings include:
- acute hospital pharmacy, wards, dispensaries, technical service (aseptic) units
- community pharmacy
- primary care - GP surgeries, care homes
- health and justice settings
- mental health settings
- community services
Initial training
Pre-registration trainee pharmacy technicians undertake a 2-year training programme and must achieve GPhC -approved education that meets the 2017 initial education and training standards. The underpinning curricula as a minimum includes:
- microbiology
- action and uses of medicines
- pharmaceutics
- pharmacy production
- professional practice
- ethical decision-making
- medicines optimisation
- accuracy-checking
Pharmacy technician training involves the completion of combined knowledge and competence-based qualifications or courses. The GPhC accredits and recognises these courses and qualifications, which lead to registration. They may be delivered face to face or at a distance. Awarding bodies - Edexcel (Pearson), NCFE Council for Awards in Care, Health and Education, Open Awards, and the Scottish Qualifications Authority - approve courses delivered in further education colleges and NHS trusts or health boards as well as providing external verification and quality assurance of assessments. These courses and their quality assurance arrangements are ‘recognised’ by the GPhC , in contrast to programme providers (for example, delivered by Buttercups Training and the University of East Anglia) which are accredited directly by the GPhC . There are also approved apprenticeship pathways made up of qualifications and courses which are integrated in terms of the end point assessment requirement of the pharmacy technician apprenticeship standard.
Pre-registration trainee pharmacy technicians must provide evidence of having completed a minimum of 2 years relevant work-based experience in the UK as part of the GPhC registration criteria. This must have been under the supervision, direction or guidance of a pharmacist or pharmacy technician to whom they have been directly accountable for no less than 14 hours per week. During these 2 training years, they must have completed at least 1,260 hours of work experience (excluding sickness absence, maternity leave and holidays) and at least 315 hours of work experience in each year.
Professional regulation of pharmacy technicians
The term ‘pharmacy technician’ is a protected title by law. All pharmacy technicians, whether working in the NHS, private or voluntary sectors in England, Wales and Scotland, must be registered with the General Pharmaceutical Council, the statutory regulator for pharmacy professionals in Great Britain. In February 2023, there were 25,191 pharmacy technicians registered with the GPhC , the vast majority of whom were employed in the community pharmacy sector.
The purpose of professional regulation is to protect the public and give them assurance that they will receive safe and effective care when using pharmacy services. The GPhC sets the professional standards that all registered pharmacy technicians must meet in relation to their education, training, conduct, performance, ethics and health. These are the minimum standards the GPhC considers necessary to protect members of the public. Registrants must meet all these standards when they first register and complete a professional declaration. Thereafter they must annually meet revalidation requirements to demonstrate continued fitness to practise.
PGDs can only be used by registered healthcare professionals who remain accountable to their professional regulator. Professional regulators have powers to take action against registrants whose practice does not comply with professional standards. An individual using a PGD must also be specifically authorised to supply and administer against that specific PGD . They are professionally accountable for each patient who is treated using a PGD and are responsible for the patient’s safety in the process. The standards set by the GPhC add an additional layer of governance to the existing protections a PGD provides, ensuring patient safety in the supply and administration of medicines.
Pharmacy technicians are not currently a registered healthcare profession in Northern Ireland. However, a public consultation on the proposal for pharmacy technicians to become regulated closed on 16 May 2022 and this policy is being progressed.
Continuing professional development and revalidation
Registered pharmacy technicians (and pharmacists) must demonstrate annually that they continue to practise both safely and effectively within their scope of practice to maintain their registration. This is known as revalidation. It is designed to demonstrate how pharmacy technicians have kept their professional skills and knowledge up to date, how they have reflected on their practice to help them improve, and how they have provided safe and effective care to patients and the public, as set out in the standards for pharmacy professionals.
To demonstrate this, pharmacy technicians must submit evidence of both planned and unplanned continuing professional development, a peer review and a reflective account. These records are reviewed on a partly targeted and partly random basis with feedback provided. A failure to meet the standards set by the regulator, or to submit their revalidation records when renewing their annual registration, may lead to the GPhC placing restrictions on a pharmacy technician’s practice and may lead to removal from the register. The GPhC will be considering any further development of the revalidation framework as part of its wider look at post-registration assurance of practice.
Association of Pharmacy Technicians UK
The Association of Pharmacy Technicians UK ( APTUK ) was established in 1952 and became the professional leadership body representing pharmacy technicians working in all sectors across the UK in 2011. APTUK provides advice, information and support to their members, advocates for and represents the profession, and enhances the education and scope of practice of pharmacy technicians.
Professional accountability of pharmacy technicians
Pharmacy technicians must ensure they provide evidence-based care within their scope of practice and competence. Should legislation be amended, when using PGDs to supply or administer medicines, they will be professionally accountable for their decisions, including actions and omissions. This also means that, even though pharmacy technicians could supply or administer a medicine legally, they are not obliged to do so and must work within GPhC standards at all times. Pharmacy technicians must have due regard to patient safety information and should be aware of, change and update their practice accordingly, which may include not using a PGD until it is amended or reviewed in light of the guidance.
Pharmacy technicians are accountable for their own practice as registrants but currently work under the direct supervision of pharmacists for the sale, supply and preparation of medicines. Supervision legislation in the Medicines Act is currently being reviewed to reflect how the profession can be enabled to provide further patient-focused clinical services to support better patient health outcomes, reflecting the registered status of pharmacy technicians in Great Britain. The Department of Health and Social Care ( DHSC ) aims to consult on legislative proposals on supervision in autumn 2023.
Safe use of PGDs
The National Institute of Clinical Excellence ( NICE ) has developed a Medicines practice guideline on the writing, authorisation, implementation and use of PGDs . They also provide a suite of tools for organisations, services and individuals to structure training and governance, and a set of standards against which organisations can monitor their performance. This guidance applies to England and Wales and is available for use in Scotland and Northern Ireland.
The NHS Specialist Pharmacy Service ( SPS ) is commissioned by NHS England to provide expert pharmaceutical support and guidance relating to all aspects of the use of PGDs through online information and national PGD templates. The information offered is publicly available and in line with NICE guidance. It is applicable to England but can also be accessed by the devolved governments.
Eligibility and training to use PGDs
NICE guidance states that appropriate training, regular re-training and assessment of competency is important for all people involved with PGDs to reduce variation and deliver safe and effective services in which PGDs are used. Competency must be assessed, and an appropriate training programme should be developed for all of those involved in considering the need for developing, authorising, using and updating PGDs .
NICE has developed and published competency frameworks for people developing, updating, authorising and using PGDs to support this guideline. Locally written training programmes may be provided by organisations for their own staff. The e-learning package written by the SPS in partnership with UK Health Security Agency ( UKHSA ) and Health Education England ( HEE ) is freely available to support healthcare professionals who use, develop, authorise, review or update PGDs to deliver services in line with legislation and NICE guidance.
Registration as a pharmacy technician does not automatically warrant use of all PGDs . Registered pharmacy technicians are required to undertake additional training as defined in each PGD to ensure only those who have been assessed as fully competent and qualified and who have completed the relevant PGD specific training may work under a PGD . This is aligned with the practice for all other healthcare professionals that can supply and administer medicines under a PGD .
Local governance of PGDs
PGDs are locally governed. Organisations already have governance arrangements in place for other professions that use PGDs , and pharmacy technicians would be expected to comply with these where the PGD is appropriate for their use. Arrangements include:
- involvement in writing and authorisation (if a new PGD is being developed or upon routine review)
- implementation of PGDs at service level
- expectation and provision of training
- assurance of competence to supply or administer the medicines included in the PGD by the service lead
- oversight of PGDs in the organisation in which staff are using them
- audits of use and impact
When developing their own PGDs , providers are required to ensure they are aware of and follow the regulatory requirements for all areas of development, authorisation and use. The NICE guideline for PGDs recommends that organisations should agree and undertake a planned programme of monitoring and evaluation of PGD use within the service. They must keep a record of all the healthcare professionals authorised to practise under the PGD . Authorised healthcare professionals must record an agreement to follow the PGD . They must provide assurances that they are trained and competent to do so.
All PGDs have clearly defined governance and education frameworks. This is quality assured by the NHS as an employer or commissioner. Healthcare professionals who will be using the PGD must be named and authorised before they use it to provide care. An appropriate member of staff - for example a GP, practice manager or lead nurse - must be responsible for authorising the healthcare professionals in each organisation. Practitioners should keep a copy of their individual authorisation and have the current authorised PGD available for reference.
Online practice and PGDs
The legal framework for PGDs does not state that an individual must be present for a supply of medicine to be made. Therefore, remote consultation prior to making a supply under a PGD is permissible and a supply can also be made in the absence of the individual themselves. The SPS has provided advice on ensuring safe care and good governance when supplying medicines remotely under a PGD .
The advice states that healthcare professionals must ensure an adequate assessment can still be conducted in a remote consultation in line with requirements for PGDs , and to the same standard as a face to face consultation. No part of the clinical assessment process, or the decision on suitability for a medicine to be supplied, can be delegated to, or undertaken by another person. Organisations must also consider how informed consent during remote consultations is obtained and documented and ensure the principles of shared decision-making are upheld.
Developing and authorising PGDs
Organisations should not develop a new PGD until they have ensured there is not one for that medicine already in use within their organisation, or in another, which they can use as a template and adapt as required. The SPS has developed PGD templates for a range of medicines, which must be clinically signed and authorised and adapted by local organisations (NHS or providing NHS commissioned services). These have been developed with experts for clinical specialties and are intended to reduce duplication and variation and improve the consistency of care.
In addition, UKHSA produces PGD templates to support national immunisation programmes provided on the NHS. In the absence of an available PGD template, NICE and the SPS have developed standard blank templates and best practice guidance on the development and authorisation of PGDs . The SPS has developed an e-learning programme in partnership with UKHSA , HEE and e-Learning for Healthcare, which is designed to support healthcare professionals who use, develop, review or update PGDs to deliver services in line with legislation and NICE guidance.
Implementation of new legislation under enabling powers
We do not expect large numbers of new PGDs to be developed specifically for use by registered pharmacy technicians. The legislative change is enabling and is more likely to be used to give registered pharmacy technicians (who complete specific PGD training and are deemed competent) the ability to use PGDs which are already utilised within an organisation, enabling them to be further utilised as part of the workforce, adding more value to multi-professional teams.
Adverse drug reactions, interactions and errors
Registered pharmacy technicians working under a PGD are expected to be able to recognise common side effects and adverse reactions to the medicines they administer and to know when there is a potential risk of an interaction. This knowledge is supported within pharmacy technicians’ initial education and training, which requires them to be able to recognise adverse drug reactions and interactions and respond appropriately. If a patient experiences an adverse reaction to a medication, once the required treatment has been undertaken, this should be recorded in the patient’s notes. The pharmacy technician should notify the Medicines and Healthcare products Regulatory Agency via the Yellow Card scheme, where appropriate.
If an error in supply or administration occurs while using PGDs , pharmacy technicians must take immediate action to manage the effects on the patient and mitigate potential side effects to the patient, and must report the error as soon as possible according to local protocols. The reporting of errors must be in an open and transparent way so that anything learned from the incident is shared as appropriate.
Human Medicines Regulations 2012
The HMRs set out a comprehensive regime for the authorisation of medicinal products, including the sale, supply and administration of medicines. The powers which allow registered healthcare professionals to sell, supply and/or administer medicines to patients using PGDs are contained in part 12 when read with schedule 16 of the HMRs .
Medicines regulation is a reserved matter (to the UK Parliament) in relation to Scotland and Wales. It is a transferred matter in Northern Ireland, which is why changes to the UK-wide HMRs that affect Northern Ireland and made under the MMD Act 2021, are made by the UK and Northern Ireland ministers. This consultation is being conducted in the names of the Secretary of State for Health and Social Care (in so far as they relate to England and Wales and Scotland) and with the Department of Health in Northern Ireland (in so far as they relate to Northern Ireland). At present, Northern Ireland pharmacy technicians are not registered and will not come within the scope of pharmacy technicians who can use PGDs until the time they are registered. However, once pharmacy technicians in Northern Ireland become a registered healthcare profession, a further amendment to the HMRs may be made so they can use PGDs also.
Legal duties
The general equality duty that is set out in the Equality Act 2010 requires public authorities, in the exercise of their functions, to have due regard to the need to:
- eliminate unlawful discrimination, harassment and victimisation and other conduct prohibited by the act
- advance equality of opportunity between people who share a protected characteristic and those who do not
- foster good relations between people who share a protected characteristic and those who do not
We do not consider this proposal to have any differential negative impacts on individuals with protected characteristics. If a patient can be assessed and any supply and/or administration can be made safely under a PGD without redirecting them to another prescriber, then this policy has the ability to remove barriers to patients in receiving the care and support they need, including the elimination of unlawful discrimination and fostering good relationships by increasing access to clinical services in the community.
This proposal has the potential to help community pharmacy deliver more patient-facing clinical services, further integrating them into the NHS and allowing them to become the first contact for minor self-limiting illnesses. This may advance equality of opportunity as it could provide more local and convenient access to medicines and a greater choice of professionals with which patients can discuss their treatment.
The National Health Service Act 2006 contains a number of overarching duties on the Secretary of State for Health which apply to every action undertaken in relation to the NHS and public health. These duties include:
- the duty to continue to promote a comprehensive health service in England (section 1)
We believe this proposal supports the duty to promote a comprehensive health service in England as it supports utilisation of the skills of the whole pharmacy team, allowing them to maximise their contribution in the provision of clinical services. The use of PGDs by registered pharmacy technicians means that certain clinical services can be offered without requiring a pharmacist or other prescribing professional to supply and administer medicines themselves or to assess the patient and write a PSD . This will free up pharmacists’ time which could be used to focus their clinical expertise on treating more complex cases as independent prescribers. This is pertinent as initial education and training reforms for pharmacists will see pharmacists become independent prescribers from the point of registration from 2026 onwards.
- the duty as to improvement in quality of services (section 1A)
We believe this also contributes to improvement in the quality of services via facilitating timely access to medicines. The ability for additional healthcare professionals to supply and/or administer medicines where it is safe and appropriate to do so will provide patients with more options for receiving the right treatment, at the right time, reducing delay. This will contribute to better patient outcomes by better using the skill mix within healthcare professions to provide additional capacity to treat patients providing new routes for access to pharmaceutical services.
Under current legislation, the only mechanism by which registered pharmacy technicians can supply and administer medicines is where they are authorised to do so by a PSD . As registered healthcare professionals, this does not fully utilise the skills and knowledge of registered pharmacy technicians who could use their education and training to supply and administer medicines safely under a PGD . If PGDs were in place, registered pharmacy technicians could administer specific medicines under an appropriate PGD without requiring the intervention of trained prescribers. This will enable registered pharmacy technicians to take responsibility for their decision to administer and supply medicines in accordance with the written PGD .
- the duty as to reducing inequalities (section 1C)
PGDs provide a structured framework which permits certain healthcare professionals to supply and/or administer medicines to a pre-defined group of patients. Increasing the accessibility of medicines for those within the defined patient group could help free capacity for appointments within other parts of the healthcare system. Any patient that falls outside the pre-defined group cannot be treated under that PGD and must be referred to an independent prescriber for an individual assessment.
Consultation questions
Do you agree or disagree with the proposal to amend the Human Medicines Regulations (2012) to enable pharmacy technicians to supply and administer medicines to patients using PGDs ?
If you have any additional information to support your answer, please provide details (maximum 150 words).
Do you agree or disagree that the 2-year pre-registration training equips pharmacy technicians with the appropriate knowledge and skills to complete the training requirements which allow them to use PGDs ?
Do you agree or disagree that allowing pharmacy technicians to supply and/or administer under a PGD will enable safe access to medicines for patients?
This proposal is to allow registered pharmacy technicians to supply and administer medicines using a PGD .
Do you have additional information in support of this proposal? (maximum 150 words)
Do you have additional information for why this proposal should not go ahead? (maximum 150 words)
Do you agree or disagree that the consultation stage impact assessment gives a realistic indication of the likely costs, benefits and risks of the proposal?
NI respondents: equality and rural screening
In Northern Ireland new policies must be screened under Section 75 of the Northern Ireland Act 1998 , which places a statutory duty on public authorities to mainstream equality in all its functions so that equality of opportunity and good relations are central to policy-making and service delivery. In addition, new or revised policies must be rural-proofed in line with the Rural Needs Act (NI) 2016 , which requires public authorities to have due regard to rural needs.
We do not consider that our proposals risk impacting different people differently with reference to their protected characteristics or where they live in NI.
If you agree or disagree, we welcome views on this point (maximum 150 words).
Do you agree or disagree that our proposals risk impacting different people differently with reference to their protected characteristics or where they live in NI?
If you agree or disagree and have evidence to support your answer, please provide details (maximum 150 words).
Do you agree or disagree that the proposal risks impacting people differently with reference to their (or could impact adversely on any of the) protected characteristics covered by the public sector equality duty set out in section 149 of the Equality Act 2010 or by section 75 of the Northern Ireland Act 1998?
Please explain your answer (maximum 150 words).
How to respond
The government invites responses on the specific questions raised. The questions can be found in the document.
Please respond through our online consultation survey .
If you have any queries on this consultation or require an alternative format, please email [email protected] . Do not send your consultation answers or any personal information to this email address.
If you have tried to message the mailbox since Monday 11 September, please resend your message to [email protected] .
If you do not have internet or email access, then please write to:
Prescribing Policy and Charges Team Department of Health and Social Care Floor 2, Area G, Quarry House Quarry Hill Leeds LS2 7UE
The consultation is open for a period of 6 weeks. Please submit your responses to the questions by 11:59pm on 29 September 2023.
Annex A: legal basis and assessment of the matters set out in section 2 of the Medicines and Medical Devices Act 2021
The Medicines and Medical Devices Act 2021 ( MMD Act) came into force on 11 April 2021. We propose to make legislative changes using powers in Part 2 of the MMD Act, which provides powers to make, among other things, amendments to the HMRs .
This consultation is conducted in line with the requirement to consult in section 45(1) of the MMD Act.
Section 2 of the MMD Act provides that patient safety must be the overarching objective of the appropriate authority when making regulations. Section 2 requires that when assessing whether regulations would contribute to the objective of safeguarding public health, the appropriate authority must have regard to 3 factors:
- the safety of human medicines and that the benefits of doing so outweigh any risks
- the availability of human medicines
- carry out research relating to human medicines
- conduct clinical trials
- manufacture or supply human medicines
As set out in section 2(3) of the MMD Act, where regulations under section 2(1) may have an impact on the safety of human medicines, the appropriate authority may make the regulations only if the authority considers that the benefits of doing so outweigh the risks.
The appropriate authority is the Secretary of State for Health and Social Care in relation to Great Britain and, in relation to Northern Ireland, it is the NI Department of Health and the Secretary of State jointly. The consultation obligation applies to both the Secretary of State and Northern Ireland Department of Health, and both will make the final decision on making any legislative changes under section 2(1).
Below we have assessed the proposals against each of the factors set out in section 2.
Continued monitoring of patient safety
PGDs make one named healthcare professional responsible for assessing a patient and supplying or administering a medicine to them. PGDs are useful where assessment and treatment follows a clearly predictable pattern. Within a PGD the suitability of supply and/or administration is determined by a set of instructions which directs the healthcare professional in their assessment of the patient. This is known as ‘the direction’. Any patients who fall outside of the pre-defined patient group within the PGD will be referred to an independent prescriber for an individual assessment.
PGDs are developed by multi-professional groups with extensive expertise, requiring a significant amount of time and resource to develop and implement. Once implemented, PGDs are subject to ongoing monitoring. All users of PGDs , including registered pharmacy technicians, are required to undertake additional training, as defined in each PGD , to be able to supply and administer any medicines under the relevant PGD . In addition, NICE guidelines recommend that organisations should agree and undertake a planned programme of monitoring and evaluation of PGD use within the service.
For all the reasons explained above, the likelihood of any increased risk of inappropriate administration of medicines is considered to be very low and is outweighed by the benefits of this proposal.
Increased availability of medicines and services
The policy has the potential for individuals to receive the treatment they need faster than if they needed to wait for another healthcare professional to prescribe, supply or administer the medicine they require. Allowing registered pharmacy technicians to undertake more clinical services via a PGD will also increase capacity for pharmacists to focus their clinical expertise and prescribing skills. Ultimately, this gives patients access to a wider range of services delivered by healthcare professionals with the right level of skills at the right time, supporting better patient healthcare outcomes and reducing the need for appointments in other parts of the healthcare system.
UK favourability to supply medicines
This proposal has the potential to have a positive impact on the UK being seen as a favourable place to supply medicines. It demonstrates that the UK has the adaptability to evolve its service design to meet the medicines requirements of local populations and to develop the capabilities of its healthcare professionals. The utilisation of the skills of pharmacy technicians will help to expand the range of patient-facing clinical services which can be offered within community pharmacies and enable registered pharmacy technicians to contribute more as part of multi-professional teams in other settings. This will improve safe and timely access to medicines, reducing delays in care. This demonstrates a forward-thinking approach to the provision of medicines which we believe will influence the likelihood of the UK being seen as a favourable place in which to supply human medicines.
Annex B: privacy notice
The Department of Health and Social Care ( DHSC ) is the data controller.
What personal data we collect
We will collect the following type of personal information:
- area of UK respondents are based in
- ethnic group
- field of work
- organisation details
- email address
How we use your data (purposes)
The data we collect is to inform DHSC of the demographic of respondents. The department will process your personal data in accordance with the Data Protection Act 1998 (DPA) and in most circumstances this will mean that your personal data will not be disclosed to third parties. We may need to contact you if we have had a request under the Freedom of Information Act 2000 (FOIA). We will also email you to let you know if we have published a response to the consultation.
Legal basis for processing personal data
Under the General Data Protection Regulation ( GDPR ), the lawful basis we rely on for processing this information is:
- Article 6(1)(e) UK GDPR
- Article (9)(i) UK GDPR
Data processors and other recipients of personal data
The Department of Health and Social Care is the data processor. Response data from respondents who have informed us that they are in Northern Ireland will be shared with officials from the Department of Health in Northern Ireland. The Northern Ireland dataset will be anonymised, names and email addresses will be removed and replaced with a response ID. If follow up of any of the responses is required by the Department of Health in Northern Ireland, this will be undertaken by DHSC .
International data transfers and storage locations
Any personal information collected will be stored in the UK and managed in line with DHSC ’s personal information charter.
Retention and disposal policy
We manage the information you provide in response to this consultation in accordance with DHSC ’s data protection policy. We will retain your data for 12 months after the consultation closes.
How we keep your data secure
Anyone managing and handling personal information understands that they are contractually responsible for following good data protection practice, are appropriately trained to do so, and are appropriately supervised.
Your rights as a data subject
By law, data subjects have a number of rights and this processing does not take away or reduce these rights under the EU General Data Protection Regulation (2016/679) and the UK Data Protection Act 2018.
These rights are:
- the right to get copies of information - individuals have the right to ask for a copy of any information about them that is used
- the right to get information corrected - individuals have the right to ask for any information held about them that they think is inaccurate, to be corrected
- the right to limit how the information is used - individuals have the right to ask for any of the information held about them to be restricted, for example, if they think inaccurate information is being used
- the right to object to the information being used - individuals can ask for any information held about them to not be used. However, this is not an absolute right, and continued use of the information may be necessary, with individuals being advised if this is the case
- the right to get information deleted - this is not an absolute right, and continued use of the information may be necessary, with individuals being advised if this is the case
Comments or complaints
Anyone unhappy or wishing to complain about how personal data is used as part of this programme, should contact [email protected] in the first instance or write to:
Data Protection Officer 1st Floor North 39 Victoria Street London SW1H 0EU
Anyone who is still not satisfied can complain to the Information Commissioners Office. Their website address is www.ico.org.uk and their postal address is:
Information Commissioner's Office Wycliffe House Water Lane Wilmslow Cheshire SK9 5AF
Automated decision-making or profiling
No decision will be made about individuals solely based on automated decision-making (where a decision is taken about them using an electronic system without human involvement) which has a significant impact on them.
Changes to this policy
This privacy notice is kept under regular review, and new versions will be available on our privacy notice page on our website. This privacy notice was last updated on 18 August 2023.
Is this page useful?
- Yes this page is useful
- No this page is not useful
Help us improve GOV.UK
Don’t include personal or financial information like your National Insurance number or credit card details.
To help us improve GOV.UK, we’d like to know more about your visit today. Please fill in this survey (opens in a new tab) .

IMAGES
VIDEO
COMMENTS
A PSD may be verbal or written but must be made after considering that individual patient and must constitute a clear instruction to the practice nurse or other competently trained health care professional to supply or administer the drug. PSDs can be an electronic instruction, provided that it can be linked uniquely to the patient
This includes written instruction templates for adoption. Specialist Pharmacy Service. When not to use a PGD. Understanding when PGDs are an unsuitable mechanism for the supply and/or administration of medicines ensures an alternative legal framework is applied. Specialist Pharmacy Service. Patient Group Direction use in End of Life Care.
A Patient Group Direction is a legal (written) framework that allows the supply and/or administration of a specified medicine (s), by named, authorised, registered health professionals, to a pre-defined group of patients needing prophylaxis or treatment for a condition described in the PGD, without the need for a prescription or an instruction ...
Overview. This guideline covers good practice for developing, authorising, using and updating patient group directions. It also offers advice on deciding whether a patient group direction is needed. Patient group directions allow healthcare professionals to supply and administer specified medicines to pre-defined groups of patients, without a ...
A PGD is a written instruction for the sale, supply and/or administration of medicines to groups of individuals who may not be individually identified before presenting for treatment. This means an individual can either be known to the service or have an appointment (for example, a baby immunisation clinic), or not be known in advance of ...
Patient group directions ( PGDs) are written instructions to help you supply or administer medicines to patients, usually in planned circumstances. They take a significant amount of time and ...
When buying a PGD the provider should make sure the organisation supplying the PGD has developed it in line with: regulations; national guidance; current clinical practice and; is legally able to authorise the PGD. Patient Specific Directions (PSDs) A PSD is an instruction to supply and/or administer a medicine written and signed by the prescriber.
A patient group direction (PGD) is a written instruction that allows named, authorised and registered healthcare professionals to sell, supply or administer named medicines in an identified clinical situation legally, without needing a written, patient-specific prescription from an approved prescriber. PGDs can be used by dental hygienists and ...
Patient Group Directives. The legal definition of a patient group directive (PGD) is 'a written instruction for the supply and/or administration of a licensed medicine or medicines in an identified clinical situation, signed by a doctor or dentist and a pharmacist'. It applies to groups of patients who may not be individually identified ...
A PGD may be used but see Patient Group Directions (NICE Guideline MPG2) (2017) Recommendation 1.1.10 before proceeding. No Yes No A PGD may be used Is the PGD to be used for managing long-term conditions, such as hypertension or diabetes, or when uncertainty remains about the Recommendation differential diagnosis? A PGD should not be used.
Whilst not defined in legislation a Patient Specific Direction (PSD) is the traditional written instruction, signed by a prescriber for medicines to be supplied and/or administered to a named individual after the prescriber has assessed that individual on a one-to-one basis. ... Understand what a Patient Group Direction (PGD) is and how it is ...
A PGD must not be confused with a Written Direction which must be patient specific. In most cases, the most appropriate clinical care will be provided on an individual basis by a specific prescriber to a specific individual patient. PGDs for the supply and/or administration of medicines should only be considered where it would offer a benefit ...
A Patient Specific Direction is a written instruction from a doctor or dentist or other independent prescriber for a medicine to be supplied or administered to a named patient. For example: ... Where a PGD is for an implant in an adult then all PGD documentation in a patient's clinical record must be kept for 10 years. For example this would ...
Draft for consultation Patient Group Directions: Good practice guidance DRAFT (April 2013) Page 5 of 74 1 This guidance does not include shared practice examples or other 2 approaches for implementing the good practice recommendations. 3 1.4 Definition of a Patient Group Direction 4 A PGD is defined in Health Service Circular (HSC 2000/026) as: 5 'A written instruction for the supply or ...
A written instruction is different to a PGD and is an arrangement between the named registered professional administering the vaccine and the authorising doctor and is subject to different legislative framework. Covid-19 vaccines cannot currently be administered via written instruction.
• Patient Specific Directions (PSDs) - written instructions, signed by a doctor, dentist, or non-medical prescriber for a medicine to be supplied and/or administered to a named patient after the prescriber has assessed the patient on an individual basis. Writing a PSD is a form of prescribing. • Patient Group Directions (PGDs).
The PGD is an option where a specified registered healthcare professional is working without the clinical supervision of a doctor, nurse or pharmacist which is a requirement of the National Protocol. ... A written instruction is not the correct mechanism for the provision of COVID-19 vaccination to health and social care staff.
A Patient Specific Direction (PSD) is the traditional written instruction, signed by a doctor, dentist, or non-medical prescriber for medicines to be supplied and/or administered to a named patient after the prescriber has assessed the patient on an individual basis. Where a PSD exists there is no need for a PGD.
Patient Group Directions (PGD) for the supply and administration of vaccinations as part of the national immunisation schedule. The legal definition of a PGD is "a written instruction for the supply and/or administration of a licensed medicine (or medicines) in an identified clinical situation, signed by a doctor or dentist and a pharmacist".
A PGD is a written instruction that permits listed healthcare professionals to supply or administer medicines to a pre-defined group of patients. The aim of this proposal is to make it easier for ...
A written instruction is different to a PGD and is an arrangement between the named healthcare professionals as detailed above and the authorising doctor. A written instruction isn't subject to the same legislated framework of a PGD. PGDs and written instructions are not interchangeable. A written instruction template is available from the BMA1.
The use of both Patient Specific Directions (PSDs) and Patient Group Directions (PGDs) is commonplace in primary care. This article will provide a brief overview of the two directions and highlight some similarities and differences between them. It will also provide examples of the situations where each type of direction is currently used and ...